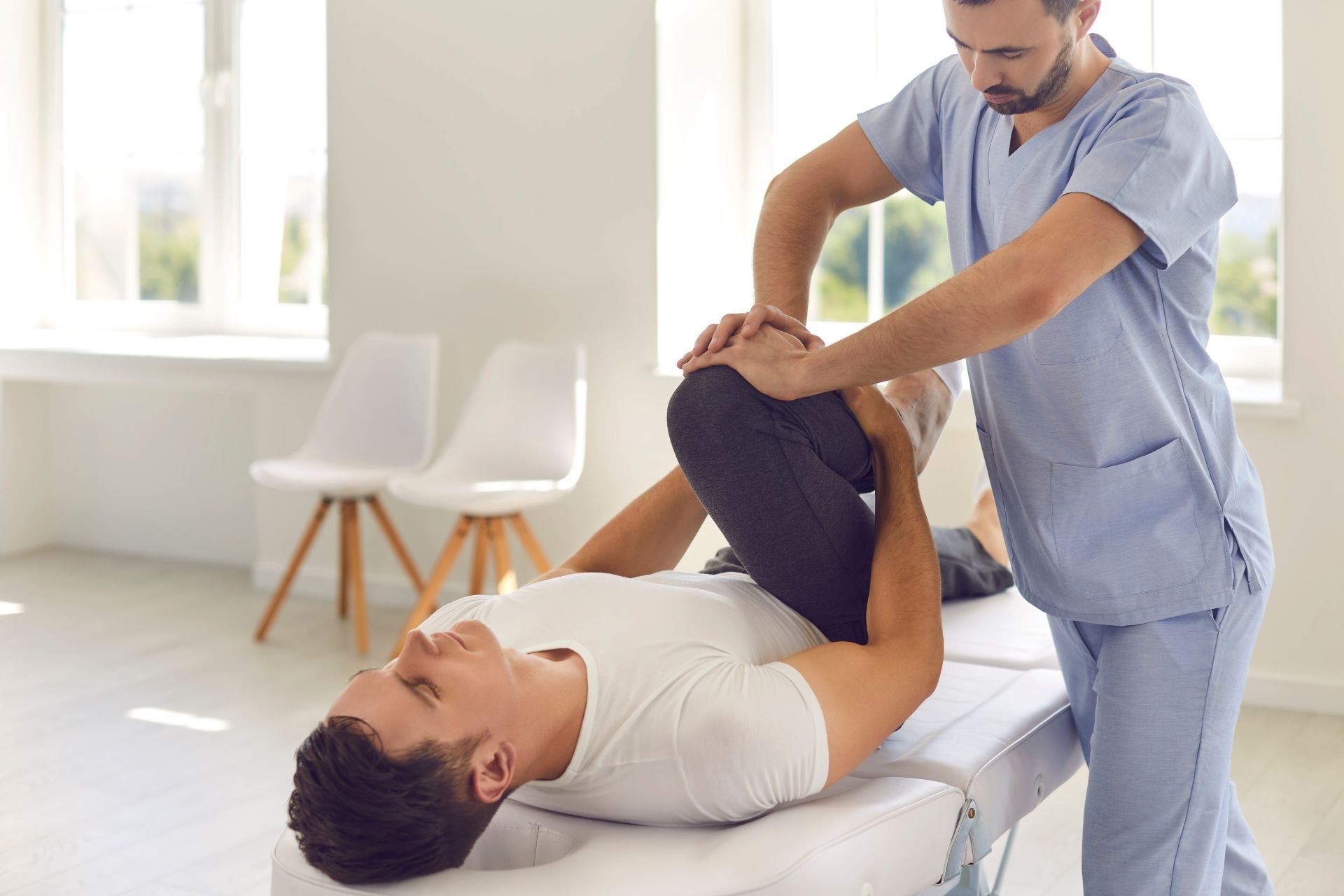
Fascial Plane Palpation
How can fascial plane palpation help in identifying restrictions in movement patterns?
Fascial plane palpation can help in identifying restrictions in movement patterns by allowing practitioners to feel for areas of increased tension, adhesions, or restrictions within the fascial planes. By palpating along the fascial planes, practitioners can detect areas of decreased mobility or areas where the fascia is adhered or restricted, which may be contributing to limitations in movement patterns. This hands-on assessment technique can provide valuable information about the quality and integrity of the fascia, helping to guide treatment strategies and interventions to address these restrictions.